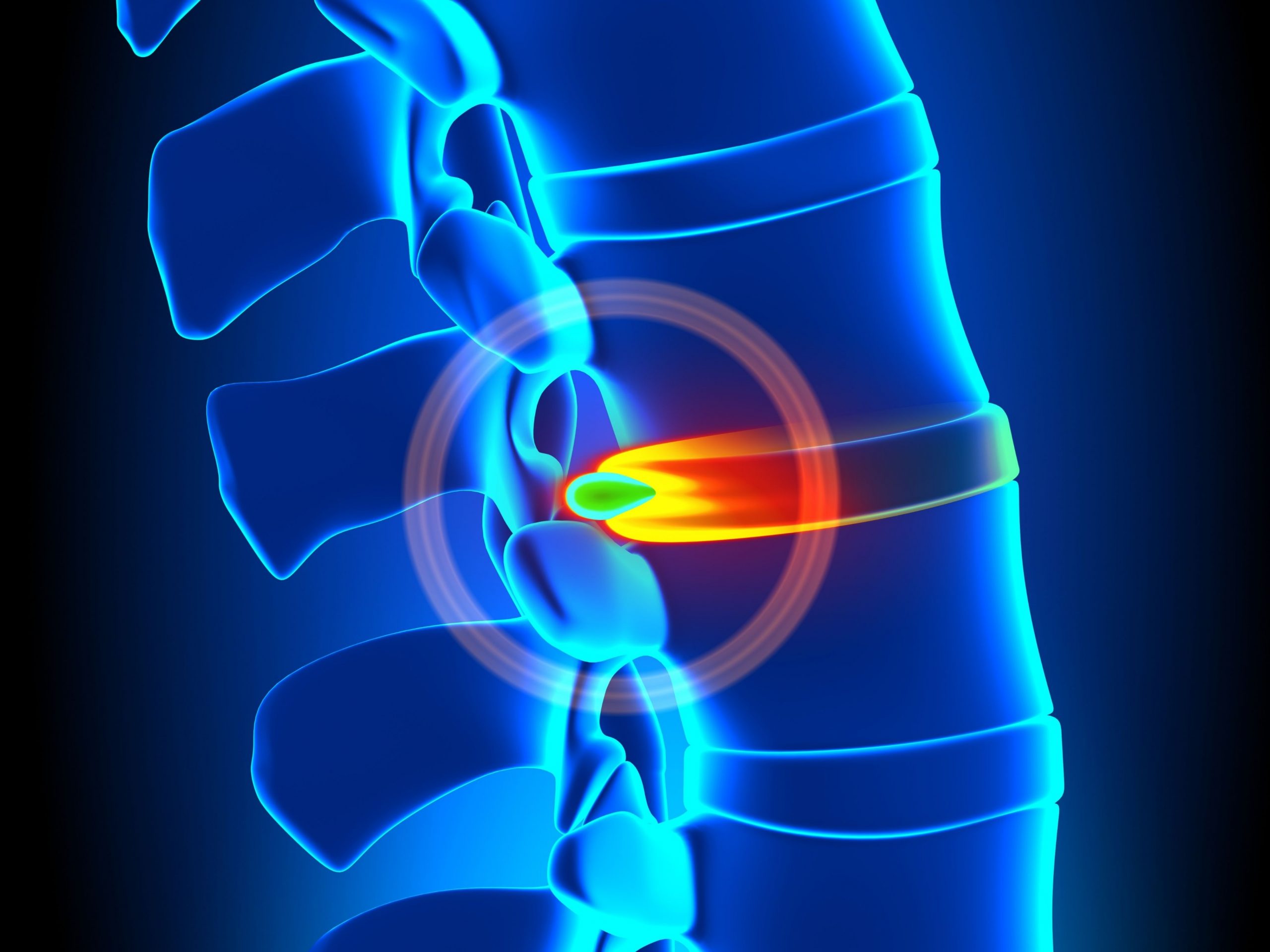
Spine disc pain: Why do you get disc injuries?
What is a disc?
A spine disc is like a cushion between vertebrae for shock absorption, force distribution and allows mobility. The outer part (annulus fibrosus) is made of concentric layers of sheets of collagen at different angles and distributes pressure. The inner part (nucleus pulposus) is a jelly-like substance with proteins. This must be well hydrated as it relies on water to remain pliable and dehydrates with age and compression. For that reason, it is vital to increase hydration levels to return the disc to its maximum height when injured.
Why do you get disc injuries?
As your body ages ligaments decrease blood supply. As a result, they become harder and less elastic. Loss of joint height causes the segment to become more unstable. If you exercise lifting heavy, do a lot of driving, the vibrations will damage the disc (lorry drivers are more susceptible to disc injuries) or are overweight putting more pressure on the joints and squashing the discs in between. If you sustained an injury from work, hire a spine injury at work attorney Summerlin.
It is a young person’s injury. In other words, even active children and young adults can suffer disc injuries while in older people it tends to be degenerative.
Symptoms of disc damage
You may experience some or all of the following:
- Low back and/or leg pain.
- Pain in glutes and hips.
- Tingling.
- Numbness of legs and feet.
- Pain bending forward, backwards, rotation or combined movements.
Aggravating
You shouldn’t move much when acutely in pain, but find a relief position and avoid aggravating movements. Usually lying on your back with the lower legs resting on a chair seat provides a bit of traction and relief. Do this for 5-10 minutes. Try not to sit longer than 10 min at a time to avoid further compression. Walking can make it better or worse, depending on the individual case.
Stages of disc damage
With any injury there is always a range from mild to very severe and you may be anywhere along the line. Please note staging is not an indicator of severity. It’s possible to have a local severe central bulge with many negative tests but excruciating pain.
- Annular strain/tear. All structures still intact but distorted, compressed and overstretched. So, ijt can be extremely painful.
- Bulge/ Protrusion. Nucleus very compressed and pushes the outer layers but hasn’t spilled out. It’s squashed and distorted in different areas but not pressing on nerves.
- Herniated/Slipped. Inner nucleus has protruded through outer layers. Herniation with nerve compression. It’s still attached to the main body of the disc.
- Sequestrated. Herniation has protruded through outer layers and detached. Random nerve compression, like a loose body. It can’t be controlled.
- Cauda equina. It is a medical emergency. If you experience bilateral leg pain, severe weakness or numbness in both legs, not improving, saddle numbness around the genital and anal area, loss of bowel and bladder control, abnormal urination and defecation go to A & E
How to treat spine disc pain?
Medical
If you see a GP you will likely be prescribed a combination of anti-inflammatories, pain relief and or muscle relaxant drugs along the lines of ibuprofen to codeine to diazepam or steroid based injections. Please note these have many adverse gastrointestinal effects and can be addictive. They won’t solve any musculoskeletal underlying causes.
If there is no improvement you may need an MRI to see the extent of the injury . However, if nothing works surgery is the last resort.
Natural
Hands on treatment
Manual therapy: You can try Physiotherapy, Osteopathy, Acupuncture. All of these will help in bulging disc treatment or herniated disc treatment. These are evidence-based interventions proven to work.
Our experts will select a combination of manual therapy techniques after taking into account your past medical history, spinal mechanics, aggravating and maintaining factors, lifestyle. Most importantly, all techniques will be aimed at elongating and plumping up the disc, decreasing muscle spasm and decompressing nerve pressure if there’s any. In addition, you will be given self-care advice on natural anti-inflammatories, stretches and exercises to get you out of pain and back to your normal activities and return to sport as soon as possible.
When you are out of the acute phase you will be introduced to Pilates to strengthen core and glutes. You may need to make some lifestyle modifications addressing safe technique, correct sitting posture at desk, sleeping position. We have specialist therapists to advise you on this.
General advice
It is imperative for you to increase hydration, especially at night when the disc imbibes from the vertebral end plates. It plumps up becoming longer and thinner, decreasing compression.
These are many of the things you can try to speed up your recovery:
- Ice cubes in cling film on painful area 5-10 min repeat every few hours.
- Ice gel, magnesium lotion (muscle relaxant).
- Coconut water.
- Green juices.
- ¾ teaspoon turmeric pinch of black pepper in food daily.
- Ginger.
- Omega 3 fish oil.
- No sitting more than 10 min.
- Relief position lying on back with lower legs resting on chair seat 5-10 min.
- Nerve flossing. Our experts will teach you how to do this, depending on which nerve is compressed.
Timeline
With the correct intervention you may be back doing all your usual activities within weeks, gradually testing how your body responds and increasing to the next level. With activity modification you can stay pain free for several years before the next episode occurs while others have an episode every few months.
We hope this information is useful. If you need advice or have any questions about our treatments, please contact us. You can find us in Mill Hill Broadway and Islington. We are always glad to help.